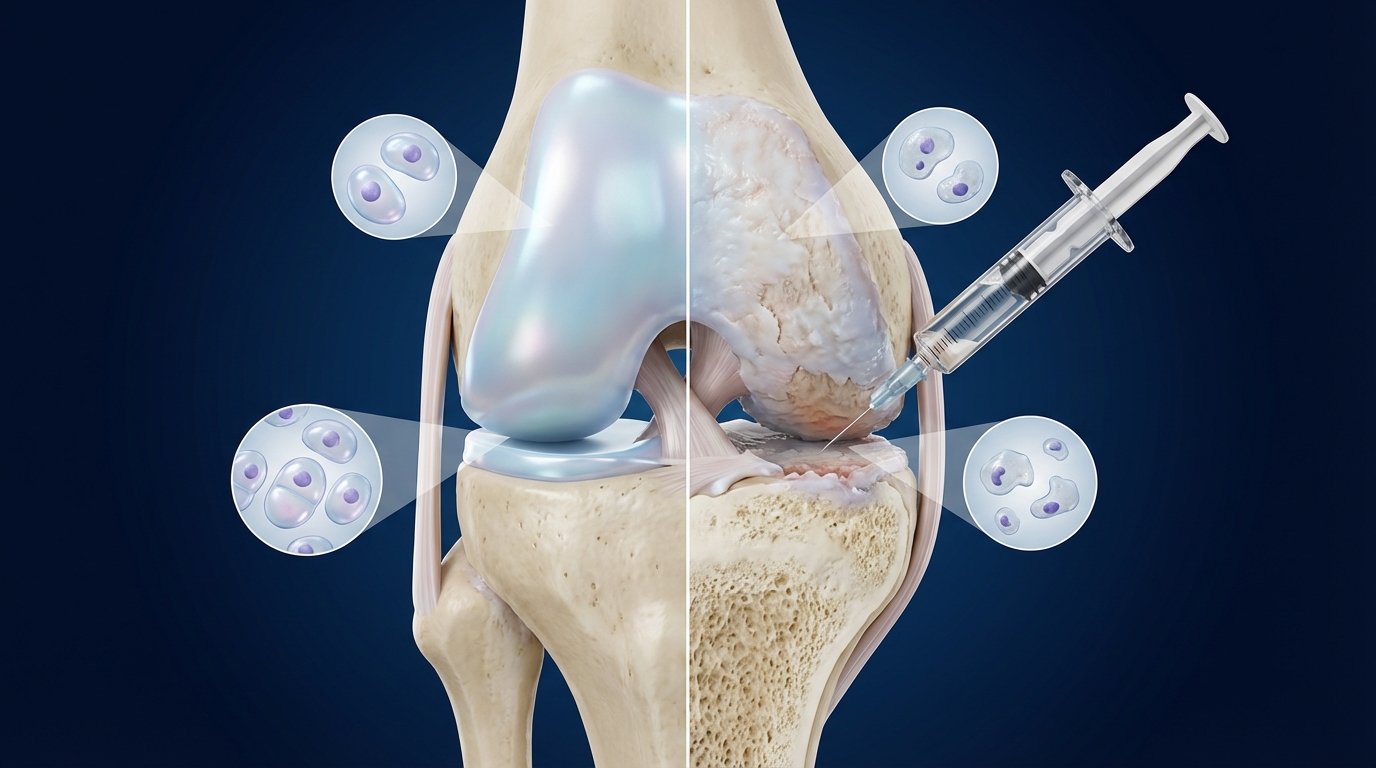
If you came to my office asking about a video from Germany that supposedly regenerates cartilage without surgery, you are not alone. In recent weeks, dozens of patients have shown me the same viral video with the same question: Doctor, is this real?
The short answer is: not the way they present it. The long answer — backed by evidence, without spin and without commercial interests — is what you will find in this article. We will review each treatment that promises to regenerate cartilage and separate what works from what is pure marketing.
The viral German video: what it claims vs. what it is
The video circulating on social media mixes two completely different products, and that confusion is part of the problem.
ChondroFiller (Meidrix Biomedicals): a collagen injectable gel applied during arthroscopy, meaning in the operating room under anesthesia. It has had CE marking in Europe since 2013 — it is not new. It is used to fill small cartilage defects but produces fibrocartilage (a repair tissue inferior to original hyaline cartilage). It works as a patch, not as true regeneration. Recovery takes 6 to 24 months.
PTK Hydrogel: a material published in Nature Communications in 2023 that showed promising results, but only in rats. It is not available for human use and years of research remain before it could be.
Facebook posts that accumulated thousands of shares claimed that a single injection regenerates cartilage in 60 days without surgery. This is false. ChondroFiller does not work that way, and PTK Hydrogel is not available for patients.
What viral videos don't tell you
ChondroFiller requires arthroscopy (surgery), produces fibrocartilage (not original cartilage), and recovery takes months, not days. PTK Hydrogel has only been tested in animals. Neither is the "miracle cure" circulating on social media.
Why doesn't cartilage regenerate on its own?
To understand why so many treatments fail, you need to understand the underlying problem. Articular cartilage is a unique tissue: it has no blood vessels, no nerves, and very few cells (chondrocytes). Think of it as an extremely smooth Teflon surface that allows bones to glide without friction.
When that "Teflon" is damaged, the body has no efficient way to repair it because blood — which carries repair cells everywhere else in the body — simply does not reach there. This is the fundamental biological reason why no injection, supplement, or alternative therapy can regenerate lost cartilage. It is a limitation of the human body, not of medicine.
Myths vs. truths: the table every patient should read
I have compiled the most common claims I hear in consultations and confronted them with available scientific evidence through 2025-2026.
| Treatment | The myth (what they sell you) | The truth (what evidence says) |
|---|---|---|
| German gel (ChondroFiller) | "Regenerates cartilage in 60 days with one injection, no surgery" | Requires arthroscopy. Produces fibrocartilage (inferior). Recovery 6-24 months. Has existed since 2013. |
| Ozone therapy | "Naturally regenerates cartilage with oxygen" | No FDA approval. No AAOS or ESSKA endorsement. "Critically low" quality evidence per 2024 umbrella review. Temporary pain relief only. |
| PRP (platelet-rich plasma) | "Your own blood regenerates your cartilage" | Does NOT regenerate cartilage. Does reduce pain in mild-moderate OA (ESSKA 2024). Effect lasts 6-12 months. Legitimate management tool, not regeneration. |
| Stem cells | "Total cellular regeneration of your joints" | Investigational. Interesting early results in small studies. No long-term data. No international medical society recommends it as standard care. |
| Hyaluronic acid injections | "Lubricates and regenerates worn cartilage" | Lubricates, yes. Regenerates? No. Pain relief for 4-6 months. AAOS does NOT recommend routine use. Useful in selected cases. |
| Oral collagen / UC-II | "Taking collagen rebuilds your cartilage" | Ingested collagen does not become articular cartilage. May reduce pain in some patients. 2025 RCT: no advantage over placebo (Scientific Reports). |
| Glucosamine + chondroitin | "Stops cartilage destruction" | Glucosamine may slow joint space narrowing (moderate evidence). Chondroitin reduces pain. Together, paradoxically, they don't work better. They don't rebuild cartilage. |
| Turmeric / omega-3 / MSM | "Natural anti-inflammatories that repair your joints" | Modestly reduce inflammation and pain. No evidence they repair or regenerate cartilage. Safe as supplements, not as primary treatment. |
| "Regenerative" diets | "Special foods that regenerate cartilage" | A balanced diet with vitamins C, D and omega-3 supports general joint health but does NOT regenerate damaged cartilage. Biologically impossible through food alone. |
Ozone therapy: very popular in Latin America, little evidence
Ozone therapy deserves special mention because in Mexico and Latin America it is extremely popular. Many clinics offer it as a "natural" treatment that regenerates cartilage using oxygen.
What does science say? An umbrella review published in Frontiers in Physiology in 2024, analyzing 8 previous systematic reviews, concluded that all had "critically low" confidence ratings. Only 3 of 8 reviews found statistically significant pain reduction compared to placebo, and ozone was not superior to other common injections like corticosteroids or hyaluronic acid.
The FDA explicitly classifies ozone as "toxic" and "irritating" with no known approved medical application. No international guideline from AAOS, ESSKA, or ACR recommends ozone therapy for osteoarthritis or cartilage repair.
PRP: what it can do (and what it can't)
Platelet-rich plasma (PRP) is probably the injectable treatment with the best available evidence, but its benefits are still more modest than advertising suggests.
A 2024 meta-analysis of 28 controlled clinical trials with 3,246 patients showed that PRP reduces pain comparably to hyaluronic acid, with superior functional improvement, especially when combined with hyaluronic acid. Leukocyte-poor PRP showed better results, particularly in mild-to-moderate osteoarthritis (Kellgren-Lawrence grades I-III).
The ESSKA ORBIT 2024 consensus endorses PRP use for early-to-moderate osteoarthritis. This is significant: a leading European medical society supports its use — but for symptom management, not cartilage regeneration.
Stem cells: promising, but still experimental
Mesenchymal stem cells (obtained from bone marrow or adipose tissue) are perhaps the most hopeful treatment in research, but we need to be honest about where we stand. Small studies have shown pain improvement and some positive MRI changes at 6-12 months. However, most studies have small sample sizes, short follow-up, and variable results.
No international medical society (AAOS, ESSKA, ACR) recommends stem cells as standard treatment for osteoarthritis or cartilage injuries. They remain investigational.
Hyaluronic acid: lubricant, not regenerator
Injected hyaluronic acid (viscosupplementation) is one of the most prescribed treatments for knee osteoarthritis. It works as a joint lubricant, not as a cartilage regenerator.
A 2024 meta-analysis with 3,851 patients (published in Pharmaceuticals) showed pain reduction at 2-4 weeks, but effects were short-lived and inconsistent. The AAOS does not recommend its routine use.
Collagen and supplements: the uncomfortable truth
I understand it is appealing to think that taking a capsule can repair a joint. Unfortunately, biology does not work that way.
Hydrolyzed collagen: when you take oral collagen, your digestive system breaks it down into amino acids — the same molecules you would get from any protein. Those amino acids do not "know" they should go to your knee, nor do they automatically assemble as cartilage.
UC-II collagen (undenatured type II): has a different mechanism, acting on the immune system. However, a 2025 randomized clinical trial with 68 patients published in Scientific Reports found that UC-II combined with hydrolyzed collagen was not superior to placebo at 12 weeks.
Glucosamine and chondroitin: a 2024 meta-analysis of 25 clinical trials showed glucosamine may slow joint space narrowing, and chondroitin reduces pain. Paradoxically, when combined — as sold in most commercial products — they did not work better than separately.
No oral supplement has been proven to regenerate articular cartilage in humans. They may be reasonable complements for pain management in some patients, but they are not substitutes for proper medical treatment.
What actually works: evidence-based surgical treatments
If cartilage does not regenerate on its own and injectable treatments or supplements do not rebuild it, then what actually works? Surgical procedures with solid evidence, indicated for focal cartilage lesions (not generalized osteoarthritis).
Microfracture
For small defects (<2 cm²). Stimulates controlled bleeding from bone to form repair tissue.
OATS (Mosaicplasty)
For medium defects (1-4 cm²). Transplant of cartilage-bone cylinders from lower-weight-bearing areas.
MACI / ACI
For large defects (>2 cm²). Implantation of the patient's own cultured chondrocytes. Strongest evidence.
Joint replacement (advanced OA)
When cartilage is completely lost. Partial or total joint replacement with robotic surgery.
| Treatment | Indication | Cartilage type produced | Evidence |
|---|---|---|---|
| Microfracture | Defects <2 cm² | Fibrocartilage (inferior) | Good (AAOS/ESSKA) |
| OATS | Defects 1-4 cm² | Hyaline cartilage (native) | Good |
| MACI/ACI | Defects >2 cm², younger patients | Hyaline-like (similar to original) | Very good (RCTs, 7+ year follow-up) |
| Robotic joint replacement | Advanced OA (grade IV) | Artificial surface | Excellent (gold standard) |
My recommendation as a surgeon
Be skeptical of any treatment that promises to regenerate cartilage without surgery, without effort, and in just weeks. If it sounds too good to be true, it probably is. Real cartilage repair requires accurate diagnosis, an individualized plan, and in many cases, a surgical procedure. There are no shortcuts in biology.
Frequently asked questions
Is it true that Germany developed a gel that regenerates cartilage?
Partially. ChondroFiller has existed since 2013 with CE marking in Europe, but it requires arthroscopy (surgery), not a simple injection. It produces fibrocartilage, an inferior repair tissue compared to original hyaline cartilage. Viral videos greatly exaggerate its capabilities.
Does PRP regenerate knee cartilage?
PRP does not regenerate lost cartilage. Meta-analyses with over 3,000 patients show it reduces pain and improves function in mild-to-moderate osteoarthritis, and ESSKA has endorsed it since 2024 for that purpose. It is a legitimate symptom management treatment, not regeneration.
Do collagen supplements help cartilage?
Oral collagen does not directly become articular cartilage. Systematic reviews show it may reduce pain and stiffness in some patients, but there is no evidence it regenerates cartilage tissue. A 2025 clinical trial in Scientific Reports found UC-II collagen was no better than placebo.
Does hyaluronic acid regenerate cartilage?
No. Injected hyaluronic acid improves joint lubrication and may reduce pain for 4 to 6 months, but it does not rebuild lost cartilage. The AAOS does not recommend its routine use. It can be helpful as a complement in selected cases of mild-to-moderate osteoarthritis.
Can stem cells repair my knee cartilage?
Mesenchymal stem cells are promising but still considered experimental. Small studies show pain improvement and some MRI changes, but long-term data is lacking. No international medical society currently recommends them as standard treatment.
What treatments actually repair cartilage?
Evidence-based surgical procedures include microfracture (small lesions), osteochondral autograft OATS (medium defects), and autologous chondrocyte implantation MACI/ACI (large lesions). These are surgical procedures endorsed by AAOS and ESSKA for focal cartilage defects, not generalized osteoarthritis.
Looking for exercises for this condition?
We have a step-by-step rehabilitation guide with illustrated exercises and an evidence-based protocol.
View rehabilitation guide: Chondromalacia →Concerned about your cartilage?
A clinical evaluation with imaging studies can determine the type and degree of your lesion, and which treatment is best for you — with no false promises.
Schedule appointment via WhatsApp