If your shoulder has slipped out of place—whether during a game, a fall, or even while reaching—it's natural to feel afraid it will happen again. It's one of the most common concerns I hear from patients here in Querétaro.
What you need to know is simple: age is the single biggest factor determining whether your shoulder will dislocate again. And that answer changes everything about what your next step should be.
What Is Shoulder Instability?
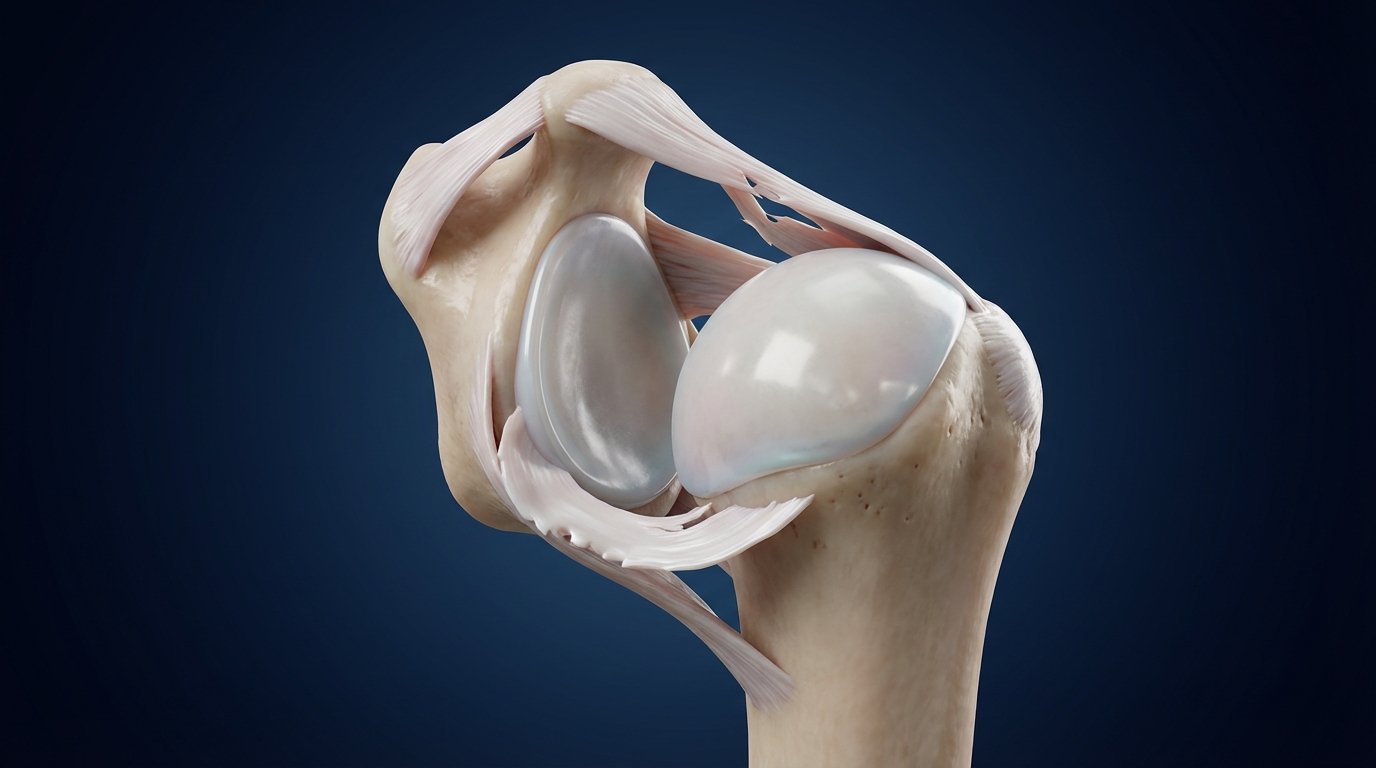
The shoulder works like a ball sitting on a pedestal. The humeral head (the ball) rests in the glenoid cavity (the pedestal), but unlike the hip, this pedestal is very shallow. Imagine a golf ball on a golf tee—that's your shoulder.
Around this joint are support structures: muscles, tendons, and the labrum, a ring of cartilage that acts as a shock absorber and increases stability. When the shoulder dislocates, this labrum frequently tears—an injury known as Bankart lesion. There can also be a dent in the humeral head called Hill-Sachs lesion.
When these structures are damaged, the joint loses stability and the risk of future dislocations increases significantly.
The most important factor: your age
The probability that your shoulder will dislocate again depends almost entirely on how old you are. This is what medicine teaches us, and why I emphasize it so much in my practice.
The Critical Data: Age Determines Risk
This is the heart of the conversation I have with every patient presenting with a shoulder dislocation. Medical studies are very clear about this, and age defines completely different strategies:
| Patient Age | Recurrence Risk (without surgery) | General Recommendation |
|---|---|---|
| Under 20 years | 90-95% | Consider early surgery |
| 20-30 years | 70-82% | Surgery recommended if active |
| 30-40 years | 45-56% | Try conservative, surgery if recurrence |
| Over 40 years | 10-15% | Conservative treatment is viable option |
Critical fact:
If you are under 25 years old and your shoulder dislocated, the probability it will dislocate again without surgery is over 80%. It's not "could happen," it's "probably will happen." This is why my recommendation is very different for my young patients.
How Is Shoulder Instability Diagnosed?
In my examination, diagnosis combines what I observe during clinical examination with imaging:
- Physical examination: Specific tests to evaluate shoulder laxity and stability (apprehension test, relocation test)
- Plain radiographs: To rule out associated fractures
- Arthrographic MRI: The gold standard for visualizing the labrum and detecting Bankart lesions
- CT scan: Useful for quantifying bone loss, especially important to decide if Latarjet procedure is needed
Conservative Treatment: When It Works
Non-surgical treatment is a valid option, but with specific conditions:
- Initial immobilization: 3 to 6 weeks in a sling
- Aggressive rehabilitation: Rotator cuff strengthening and scapular stabilizer exercises
- Activity modification: Avoiding contact sports and high-risk movements
Conservative treatment has better outcomes in patients over 40 years old, with low occupational risk, and who accept limitations in physical activity.
Surgical Treatment: Your Options
When surgery is necessary, I have two main options depending on your specific case:
Preoperative Evaluation
Quantify bone loss and assess associated injuries
Bankart Repair
Arthroscopic approach for labral lesions without major bone defects
Latarjet Procedure
For significant bone loss or engaging Hill-Sachs lesion
Rehabilitation
3-6 months of gradual recovery until return to sport
Arthroscopic Bankart Repair
This is my technique of choice for most cases. It's performed entirely arthroscopically (minimally invasive) and consists of repairing the torn labrum. Success is high: over 90% when there is no significant bone loss (less than 13.5% of the glenoid cavity).
Advantages:
- Faster recovery than open surgery
- Less postoperative pain
- Minimal scarring (only small incisions)
- High success rate
Latarjet Procedure
This procedure is recommended when there is significant bone loss in the glenoid cavity (greater than 13.5%) or when a Hill-Sachs lesion will engage during movement. In this case, I transfer a bone fragment (coracoid process) from your scapula to the shoulder cavity, increasing stability.
It's a more complex technique than simple Bankart repair, with an important learning curve, but with excellent results when indicated.
Bankart vs. Latarjet Comparison
| Aspect | Bankart Repair | Latarjet Procedure |
|---|---|---|
| Primary indication | Bankart lesion, bone loss <13.5% | Bone loss >13.5%, Hill-Sachs engagement |
| Approach | Arthroscopic (minimally invasive) | Open or hybrid |
| Success rate | >90% | 93-97% |
| Recovery | 4-6 weeks (normal activity) | 6-8 weeks (normal activity) |
| Postoperative pain | Mild to moderate | Moderate |
When Should I Have Surgery? Clear Criteria
This is the question I'm asked most often, and the answer depends on several factors:
- Two or more dislocation episodes: After a second dislocation, the risk of a third is very high. Surgery is recommended.
- First episode in young patients (<30 years) with contact sports: The numbers speak for themselves: 70-95% will have another dislocation without surgery.
- Significant bone defect: If studies show major bone loss (Hill-Sachs or anterior defect), early surgery makes sense.
- Failed conservative treatment: If after 3 months of aggressive rehabilitation there is persistent instability.
My professional advice:
In young, active patients with a first dislocation, I frequently recommend early surgery because the recurrence rate without it is simply too high. It's better to have planned surgery when the patient is mentally prepared than to experience multiple new dislocations causing more damage and frustration.
Postoperative Recovery: The Timeline
Recovery after Bankart repair follows this general process:
Weeks 1-4: Immobilization and Passive Movement
- Sling for 4-6 weeks
- Gentle passive movements to maintain range
- Ice and elevation to reduce inflammation
Weeks 4-8: Active-Assisted Movement
- Beginning of active shoulder movement
- Rotator cuff strengthening
- Specialized physical therapy 3 times per week
Weeks 8-12: Active Rehabilitation
- More intense strengthening exercises
- Full range of motion work
- Advanced scapular stabilization
Weeks 12-16+: Return to Sport
- Sport-specific exercises
- Gradual intensity progression
- Complete return between 4-6 months in most cases
Frequently Asked Questions
How many times does the shoulder have to dislocate before surgery is needed?
Recommendations have evolved. Previously, we waited for 2-3 dislocations before operating. Today, after a first dislocation in an active young patient (under 30), early surgery is a valid option because it prevents recurrences, additional damage, and the frustration of multiple episodes. In older patients, conservative treatment is more viable.
Can you live with an unstable shoulder without surgery?
Technically yes, but with limitations. You must accept that certain movements are contraindicated, contact sports are risky, and fear of another dislocation may affect your quality of life. In patients over 40 with low activity, it is an option. In young active patients, it is generally not advisable.
How long does Bankart repair surgery take?
Arthroscopic Bankart repair typically takes between 45 minutes and 1.5 hours, depending on injury complexity. Latarjet procedure can take 90 minutes to 2 hours.
Can I return to sports after surgery?
Yes, most of my patients return to their usual sport between 4-6 months after surgery, as long as they complete appropriate rehabilitation. Contact sports require more aggressive rehabilitation. The key is strict adherence to the physical therapy program.
What happens if I don't have surgery and the shoulder keeps dislocating?
Each recurrent dislocation causes additional damage: further labral tearing, increased Hill-Sachs lesions, possible fracture. This makes eventual surgery more complex. Additionally, the risk of shoulder arthritis increases with each episode. Planned surgery is better than multiple dislocations causing progressive damage.
Does arthroscopic surgery leave a scar?
The advantage of arthroscopy is that it leaves only 3-4 small incisions (5-10 mm each). Scars are minimal, almost invisible after a few months, especially compared to open surgery which would require a 5-7 cm incision.
Did you have a shoulder dislocation?
I personally evaluate your case and clearly explain your options regarding shoulder instability and dislocation.
Schedule appointment via WhatsApp