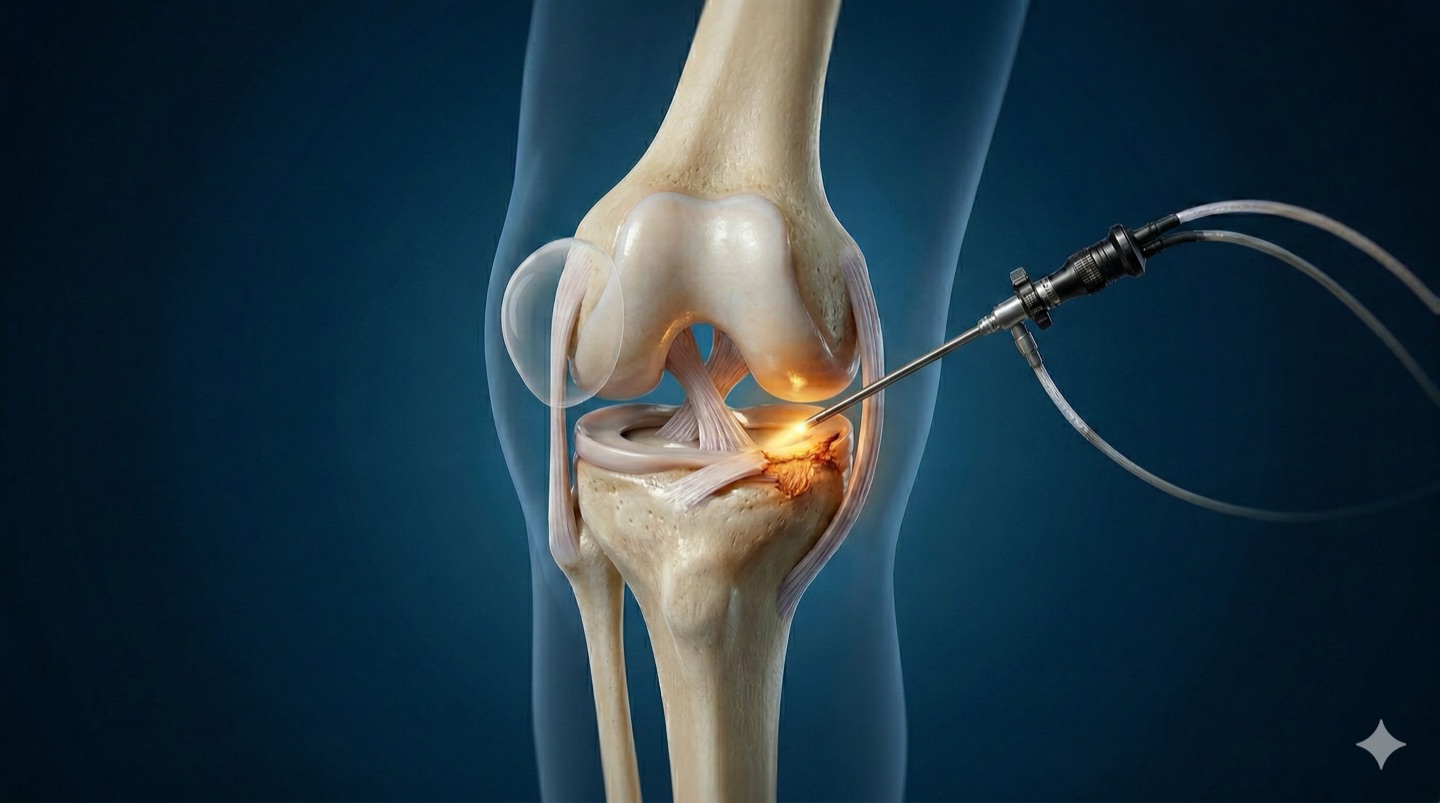
If you have been diagnosed with a meniscus tear or a cartilage injury in your knee, it is normal to feel uncertain. Do you need surgery? How long is the recovery? Will you be able to return to sports? In this guide, I explain step by step what knee arthroscopy is, when it is recommended, what treatment options exist, and what to expect after surgery.
Why Queretaro?
Located 2.5 hours from Mexico City and 45 minutes from San Miguel de Allende, Queretaro offers world-class private hospitals at a fraction of U.S. costs. I perform knee arthroscopy at modern, fully equipped surgical centers using the same techniques and implant systems available in leading U.S. and European hospitals. English-speaking staff, written quotes, and insurance coordination are standard for our international patients.
What is knee arthroscopy?
Arthroscopy is a minimally invasive surgery that allows the surgeon to see and treat the inside of the knee without opening it. A high-definition camera called an arthroscope (only 4 mm in diameter) is inserted through incisions approximately 5 mm long. Specialized instruments are introduced through a second portal to repair the injury.
Before arthroscopy existed, treating a meniscus tear required an arthrotomy (opening the knee completely), resulting in large scars, considerable pain, and weeks of immobilization. Today, arthroscopy has almost entirely replaced open surgery: it is performed on an outpatient basis, with minimal incisions and a much faster recovery.
It is the most commonly performed orthopedic surgery in the world, with millions of procedures each year. That accumulated experience has made it a safe, reproducible procedure with predictable outcomes when indicated correctly.
When is knee arthroscopy recommended?
Arthroscopy is indicated for internal knee injuries that do not respond to conservative treatment. The most common indications include:
- Meniscal tears with persistent pain, mechanical locking, or recurrent swelling
- Articular cartilage lesions (chondral and osteochondral defects)
- Loose bodies inside the joint causing locking or catching
- Symptomatic synovial plica or chronic synovitis unresponsive to medical treatment
Not every meniscus tear needs surgery
In older patients with degenerative osteoarthritis, meniscal tears are frequently an incidental finding that does not require surgical treatment. International guidelines (BMJ 2017) recommend against arthroscopy for degenerative knee disease, as it shows no benefit over conservative treatment. The key is distinguishing an acute traumatic tear (which does benefit from surgery) from a degenerative tear in a knee with osteoarthritis (which generally responds better to rehabilitation and injections).
Understanding the meniscus: why the location of the tear matters
Each knee has two menisci: the medial (inner) and the lateral (outer). They are C-shaped structures made of fibrocartilage that function as shock absorbers between the femur and tibia. They distribute load, stabilize the joint, and protect the cartilage.
What many patients do not know is that the meniscus does not have the same blood supply throughout its entire structure. Think of a sponge that dries from the center outward: the outer portion receives blood and can heal; the inner portion does not receive blood and has very little capacity to heal on its own.
Surgeons divide the meniscus into three zones based on blood supply:
- Red-red zone (periphery, outer 25-30%): good blood supply. Tears here can be repaired with sutures and have healing rates of 80-90%.
- Red-white zone (transition): variable blood supply. Sometimes repairable, depending on the tear pattern and tissue quality.
- White-white zone (inner 65-70%): no blood supply. Tears here generally do not heal with sutures and usually require partial resection.
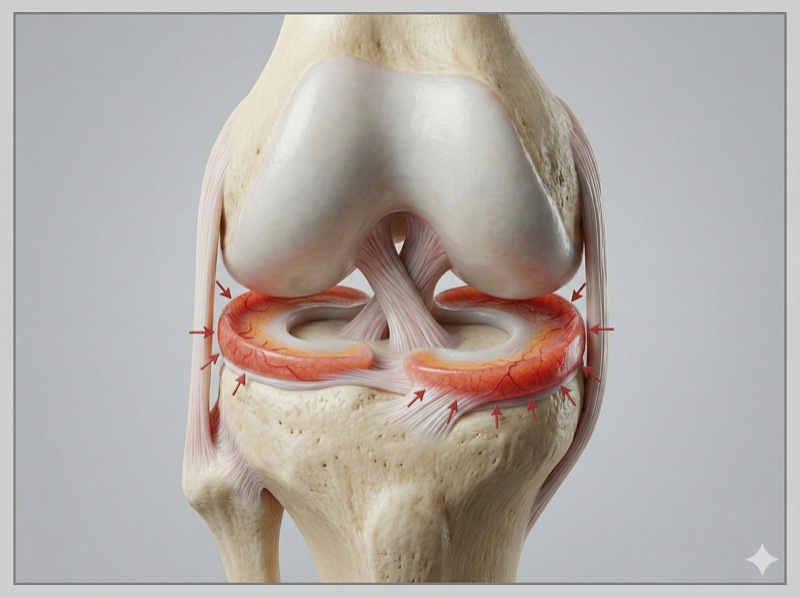
In addition to location, the tear pattern influences the decision. Vertical longitudinal tears are the most repairable (80-90% success rate in the red zone). Bucket-handle tears displace a fragment that locks the knee and require urgent repair. Horizontal, radial, or complex degenerative tears are generally not repairable and are treated with selective resection.
This is why, before operating, I explain both possible scenarios to you: repair or resection. The final decision is made in the operating room when the injury is directly visualized.
The procedure step by step
Evaluation
MRI, clinical exam, preoperative workup
Preparation
8-hour fast, companion, regional nerve blocks
Arthroscopic surgery
5 mm portals, HD camera, treatment based on findings
Discharge and recovery
Outpatient, ice, progressive rehabilitation
1. Office evaluation
Diagnosis begins with a detailed clinical examination: specific meniscal tests (McMurray, Thessaly), ligament assessment, and range-of-motion evaluation. An MRI confirms the injury and allows us to plan the approach before entering the operating room.
Preoperative studies are ordered in accordance with NOM-006-SSA3-2011, Mexico's official standard for the practice of anesthesiology: blood work, electrocardiogram, and pre-anesthetic evaluation. If you have chronic conditions, we coordinate with your internist to optimize your health before surgery.
2. Day-of-surgery preparation
Arthroscopy is performed under regional nerve blocks and mild sedation. The anesthesiology team applies targeted blocks to the nerves that provide sensation to the knee, so the surgical area is completely numb. Mild sedation keeps you relaxed and comfortable during the procedure without the need for general anesthesia or a spinal block. This allows faster anesthetic recovery, with less nausea and without the effects of a full lower-extremity block.
An 8-hour fast is required, along with a companion to drive you home after the procedure. Surgery is scheduled in the morning, and in most cases you return home the same day.
3. The arthroscopic procedure
Two to three portals (5 mm incisions) are made around the knee. A high-definition camera is introduced through one portal; surgical instruments are inserted through the others. The complete procedure takes between 30 and 60 minutes, depending on the complexity of the injury.
Once inside, I directly assess the menisci, cartilage, ligaments, and synovium. Based on the findings, I perform the most appropriate treatment: meniscus repair with all-inside technique, selective partial meniscectomy, microfractures, or osteochondral autograft transfer (OATS) for cartilage lesions.
4. Discharge and immediate recovery
Arthroscopy is an outpatient procedure: you go home the same day. Immediate instructions include local ice application, leg elevation, pain and anti-inflammatory medications, and isometric exercises starting within the first few hours. Formal rehabilitation begins in the following days and is tailored to the type of procedure performed.
Meniscus repair vs. meniscectomy: why preserving the meniscus matters
This is probably the most important decision during a knee arthroscopy. When I encounter a meniscal tear, the first question is always: can it be repaired?
My philosophy is clear: repair before resection. And the reason is compelling: long-term studies show that meniscectomy (even partial) significantly increases the risk of osteoarthritis. At 21 years of follow-up, up to 48% of patients who underwent meniscectomy develop osteoarthritis, compared with only 7% in healthy controls. The meniscus is not a dispensable tissue.
| Aspect | Meniscus repair | Partial meniscectomy |
|---|---|---|
| Initial recovery | Slower (crutches 4-6 weeks) | Fast (walk the same day) |
| Weight-bearing | Partial with crutches 4-6 weeks | Full immediate |
| Return to sports | 5-9 months | 4-8 weeks |
| Long-term osteoarthritis risk | Significantly lower (~21%) | Elevated (~51%) |
| Success rate | 80-87% at 5 years | Immediate relief in >90% |
Meniscus repair is not always possible. It depends on the tear zone, the pattern, tissue quality, and the patient's age. But when it is viable, the long-term benefits far outweigh a slower recovery. After a meniscectomy, the load on the cartilage increases by 50 to 70%, which accelerates joint wear.
A repaired meniscus is worth the wait
Recovery after a meniscus repair is slower than after a meniscectomy: crutches for several weeks and return to sports in months, not weeks. But in the long run, preserving the meniscus protects the joint against osteoarthritis. It is an investment in your knee's health for the next 20 years.
For international patients
I regularly treat expats and visitors from the U.S. and Canada living in Queretaro and San Miguel de Allende. Here is what you should know:
- Communication: I speak English and all pre-op instructions, consent forms, and post-op care plans can be provided in English
- Cost: Knee arthroscopy in Queretaro costs a fraction of what you would pay in the U.S. — even without insurance. We provide a written quote before surgery
- Insurance: We work with major Mexican private insurance carriers. If you have international or U.S.-based insurance, we can provide documentation for reimbursement
- Follow-up: We coordinate post-operative rehabilitation locally and can share records with your physician back home
Frequently asked questions
Can I walk after knee arthroscopy?
It depends on the procedure performed. After a partial meniscectomy, most patients walk the same day with full weight-bearing. After a meniscus repair, crutches with partial weight-bearing are used for 4-6 weeks to protect the repair. Cartilage procedures (microfractures, OATS) require weight-bearing restrictions for 6-8 weeks. In all cases, the rehabilitation team guides you step by step.
How does the surgeon know if my meniscus can be repaired?
Three factors are evaluated during surgery: the location of the tear (zones with better blood supply heal better), the tear pattern (vertical longitudinal tears are the most repairable), and tissue quality (a degenerative meniscus does not hold sutures well). The final decision is made in real time, by directly visualizing the injury with the arthroscopic camera.
Is it true that arthroscopy does not work for osteoarthritis?
For degenerative knee disease (osteoarthritis), scientific evidence shows that arthroscopy offers no benefit over conservative treatment. Landmark studies and international guidelines (BMJ 2017) recommend against arthroscopy for degenerative knee osteoarthritis. However, arthroscopy remains highly effective for acute traumatic injuries: meniscal tears in young patients, sports injuries, and cartilage lesions. The key is distinguishing between a degenerative tear and a traumatic tear.
How much does knee arthroscopy cost?
The cost varies depending on the hospital and the complexity of the procedure (a simple meniscectomy is not the same as a meniscus repair with cartilage restoration). Arthroscopy is covered by most major medical insurance plans. At your consultation we provide a written quote and assist you with insurance authorization paperwork.
How much time off work will I need?
For office work: 1-2 weeks after meniscectomy, 2-4 weeks after meniscus repair. For physical work: 3-5 weeks after meniscectomy, 6-8 weeks after meniscus repair. These timelines are approximate and are adjusted based on each patient's progress. We provide documented medical leave for your employer or insurance company.
Looking for exercises for this condition?
We have a step-by-step rehabilitation guide with illustrated exercises and an evidence-based protocol.
View rehabilitation guide: Partial Meniscectomy →Knee pain or a meniscal injury?
We will evaluate your case to determine the best treatment. Written quote provided. English-speaking staff.
Schedule evaluation via WhatsApp